
CBT for Overcoming Self-Doubt | A Practical Guide to Breaking the Loop
If you are looking into overcoming self-doubt, CBT offers a practical way to understand why the loop keeps coming back and what helps loosen its grip. Self-doubt can look quiet from the outside. You may second-guess an email, replay a conversation, hold back from speaking, or ask someone else what they think before trusting your own view. At times, that may seem sensible. But when it becomes repetitive, it often starts to shrink your confidence instead of protecting it.
From a CBT point of view, self-doubt is rarely just one thought. It is usually a cycle. Something triggers uncertainty, your mind makes a negative prediction, anxiety or tension rises, and you do something to feel safer. That might be overthinking, reassurance-seeking, avoiding action, or aiming for impossible standards. As explained in the guide to cognitive behavioural therapy, and in Therapy For Me ‘s work, the aim is not to force confidence. It is to understand the pattern clearly enough that you can respond to it differently.
What Self-Doubt Can Look Like in Everyday Life
Self-doubt is a pattern of questioning your own judgement, ability, or worth. It can show up at work, in relationships, socially, in parenting, in study, or in ordinary day-to-day decisions. The content may change, but the feeling underneath is often similar. You are not sure whether to trust yourself, and the mind keeps pushing for more certainty before you act.
When self-doubt goes beyond occasional uncertainty
Most people question themselves sometimes. That is part of being human. A pause before a big decision or a wobble after a difficult moment does not automatically mean you are stuck in a harmful cycle.
The pattern becomes more difficult when doubt starts showing up again and again, even in situations you usually handle well. You may feel unable to let a decision stand, unsure whether your judgment counts, or overly affected by the possibility of getting something wrong. Instead of helping you reflect and move on, doubt keeps pulling you back into review.
Common signs the loop is active
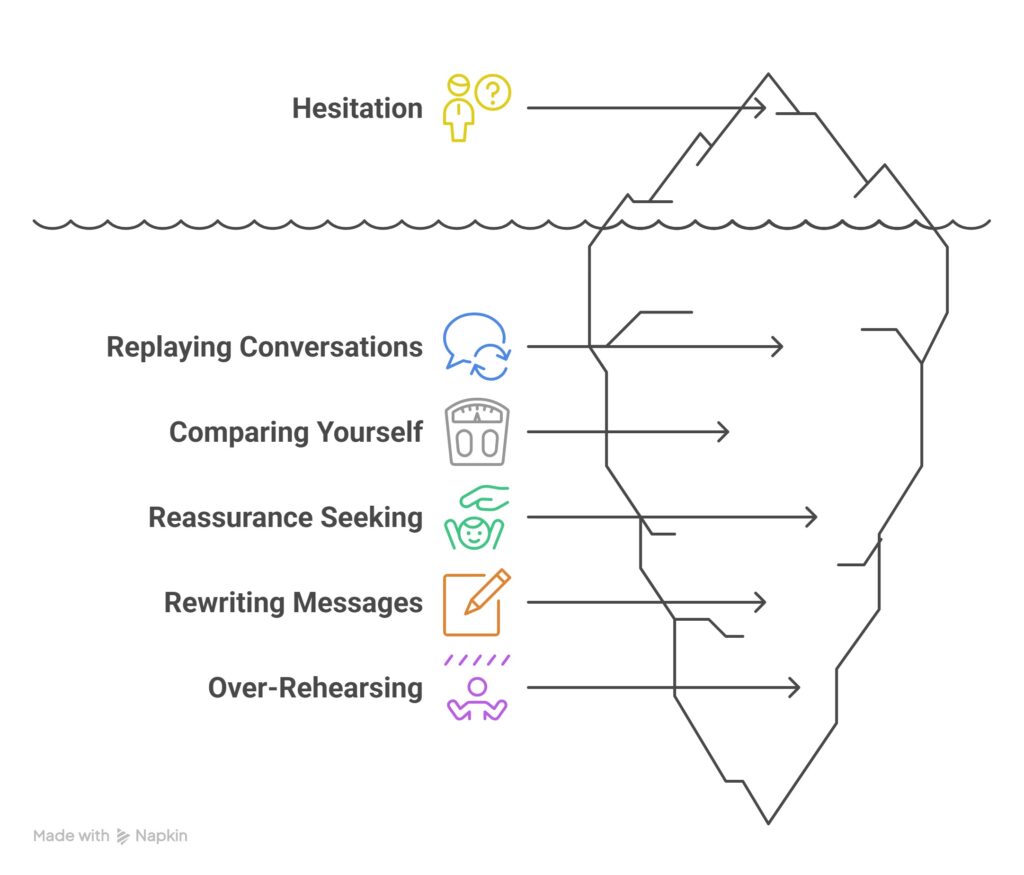
You may notice that you replay conversations after they have finished, compare yourself with other people, ask for reassurance before trusting your own view, or put off action until you feel more certain. Some people start rewriting messages, changing decisions, or mentally rehearsing what they will say before speaking up.
These habits are understandable. But over time they can train you to treat hesitation as proof that you are not ready.
What Triggers Self-Doubt
Self-doubt usually gets activated in situations where something feels meaningful or uncertain. What matters most is often the meaning your mind attaches to the situation.
Fear of getting things wrong
For many people, self-doubt is triggered by the possibility of making a mistake. That might happen at work when you create or present something important, in a relationship when you are unsure how you came across, or in everyday life when you have to make a decision not knowing whether it is the best one.
The mind can quickly jump from “I might get this wrong” to “If I get this wrong, it means something bad about me.” Once that shift happens, the situation starts to carry extra emotional weight, which is one reason overcoming self-doubt can feel difficult when fear of mistakes and fear of experiencing regret is running the show.
Comparison and fear of judgment
Self-doubt also grows easily in situations where you compare yourself to other people. You may assume they are coping better, speaking more confidently, or getting things right with less effort. That can leave you feeling behind before anything has even happened.
For some people, the trigger is not comparison itself but imagined judgment. You may worry that other people will notice your hesitation, think less of you, or decide you are not capable. That can make even ordinary tasks feel more loaded than they need to be.
Uncertainty and not knowing how things will go
Uncertainty is one of the strongest triggers in this cycle. When you do not know how something will go, your mind may treat that lack of certainty as a problem that must be solved before you act. That is one reason self-doubt can feel so sticky. Real life rarely gives complete reassurance in advance.
A similar pattern can show up around physical symptoms too, which is why Therapy For Me’s blog on CBT for health anxiety may be useful if uncertainty about health is one of the areas that triggers doubt for you.
What Keeps the Self-Doubt Cycle Going
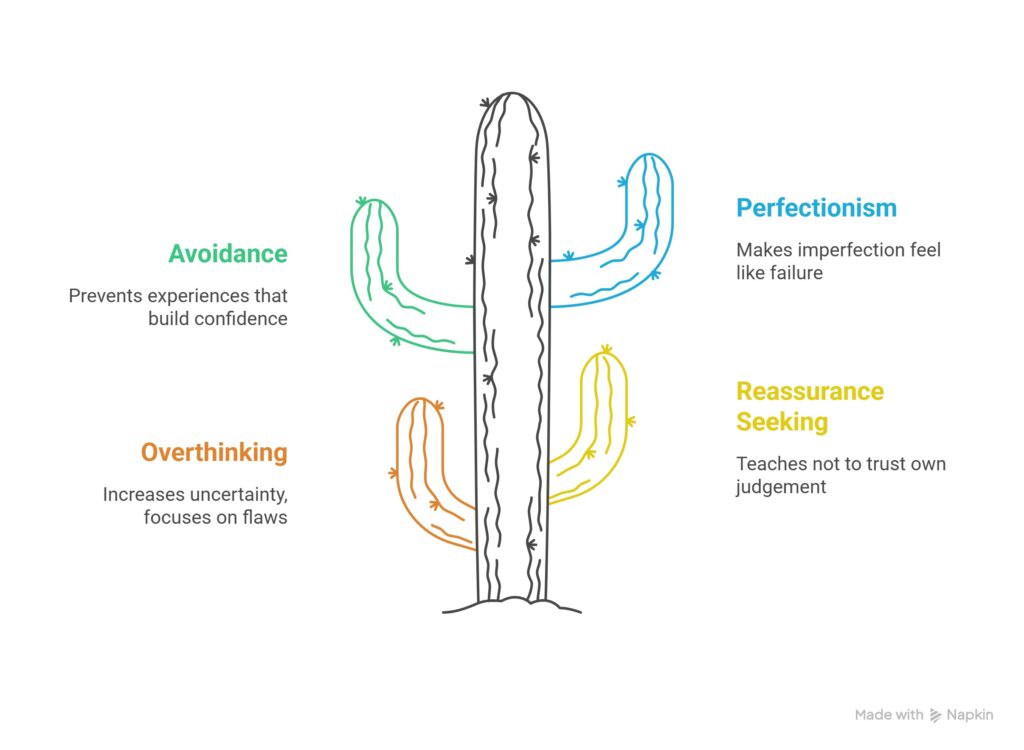
The self-doubt cycle often gets maintained by the ways you respond to cope with it. These responses usually make sense in the moment. They reduce discomfort, help you feel more prepared, or protect you from feeling exposed. The problem is that they also stop you learning that you may be more capable than the doubt suggests.
This fits with how the NHS describes CBT, as a therapy that helps you change how you think and act. In the self-doubt cycle, avoidant and safety-seeking habits can stop you from learning that the feared prediction may not be as accurate as it feels.
Overthinking and mental review
Overthinking can feel productive because it gives the impression that you are being careful. You go back over what you said, what you did, what you should have done, or what might happen next. But instead of bringing clarity, it often increases uncertainty. The more you review, the less settled you feel.
Mental review also keeps your attention fixed on possible flaws which leads to attention biases. Rather than noticing the bigger picture, you begin scanning for signs that you got something wrong or missed something important.
Reassurance seeking
Reassurance may come from other people or from your own mental habits. You might ask whether something sounded okay, whether you made the right choice, or whether you are overreacting. You might reread messages or look for signs that everything is fine.
This can lower anxiety for a short while. But it also teaches the mind that you cannot rely on your own view without checking first. That can strengthen self-doubt over time.
Avoidance and playing small
One of the most powerful ways self-doubt stays alive is through avoidance. You may hold back from applying for something, delay a conversation, keep your opinion to yourself, or stay in the background until you feel more confident.
The difficulty is that confidence often grows after action, not before it. If you keep waiting until doubt disappears, you may end up treating hesitation as proof that you should not try.
Perfectionism and impossible standards
Self-doubt often becomes more intense when your internal standards are too high and rigid. If your rule is that you must do things flawlessly, feel fully certain, or never look unsure, then ordinary human imperfection starts to feel like failure.
Mind’s advice on improving your self-esteem encourages people to recognise negative self-beliefs and build a kinder, more balanced view of themselves, which fits closely with CBT work around perfectionism and self-doubt.
This matters for self-doubt because perfectionism leaves very little room for learning, experimenting, or being average at something while you improve.
How CBT Understands Self-Doubt
CBT treats self-doubt not as a fixed part of your personality, but as a pattern of predictions and responses that can be understood and changed.
The prediction behind the doubt
Under self-doubt there is often a prediction. It may sound like, “If I say the wrong thing, people will see I am not good enough,” or, “If I cannot feel sure, I should not trust myself.” These predictions often arrive quickly and feel convincing, especially in situations that matter to you.
This is also why Every Mind Matters’ guide to reframing unhelpful thoughts is so relevant here. It encourages people to catch unhelpful thoughts, check them, and respond in a more balanced way. That fits closely with the self-doubt loop, where beliefs about your ability or worth shape what you do next.
Why certainty never quite feels enough
Trying to feel fully certain before you act usually backfires. You may get brief relief, but it rarely lasts. Another doubt appears, or the mind asks for one more check.
This is why CBT helps you build a different relationship with uncertainty rather than waiting for it to disappear first.
CBT for Overcoming Self-Doubt in Practice
In practice, CBT helps you slow the cycle down and respond to it in a more useful way. Rather than arguing with every doubtful thought, you learn how to notice the trigger, identify the prediction, and look at what your response is teaching you.
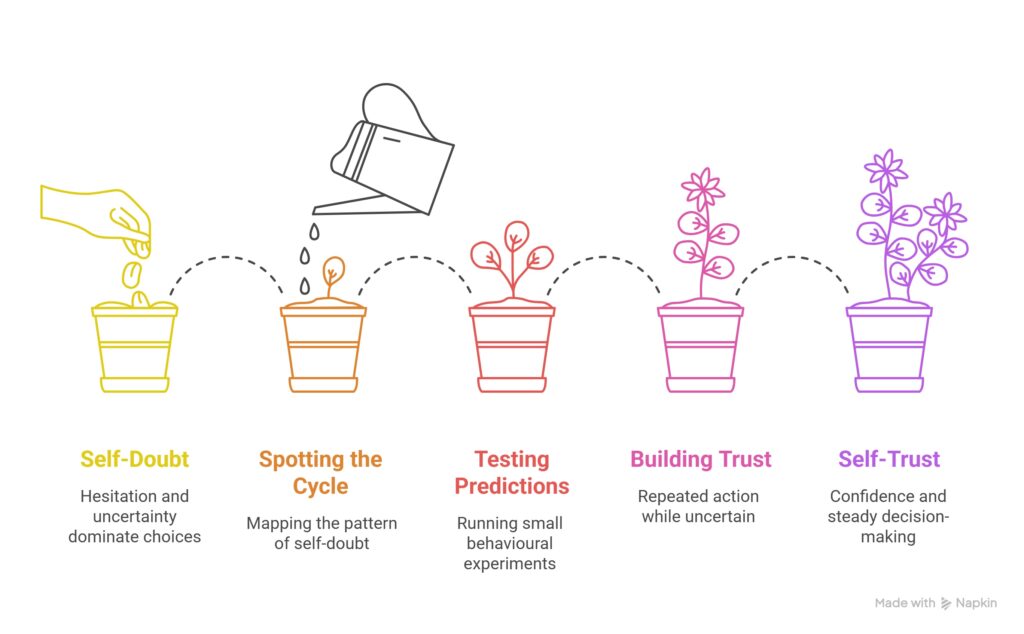
Spotting the self-doubt cycle
One of the first steps is often to map the sequence. What happened just before the doubt showed up? What did the mind predict? What feeling followed? What did you do next?
This matters because patterns become easier to change once you can see them clearly and name them. Instead of experiencing the doubt as a vague truth about who you are, you begin to recognise a process with moving parts.
Testing unhelpful predictions
A central part of CBT is testing predictions rather than automatically obeying them. If your mind says, “If I speak up, I will sound foolish,” the task is not to replace that with forced positivity. The task is to test what actually happens.
That might mean speaking briefly in a meeting without overpreparing, sending a message without checking it several times, or making a small decision without asking for reassurance. These are called behavioural experiments in CBT. They give you new information that the self-doubt cycle would otherwise block or prevent.
Building trust through small actions
Steadier self-trust usually grows through repeated action, not one big breakthrough. You do something while still feeling uncertain, notice the outcome, and learn that discomfort does not automatically mean danger or failure.
That is why overcoming self-doubt often depends less on feeling different first and more on responding differently in small, realistic ways.
Therapy for self-doubt and when support helps
Sometimes the pattern is so familiar that it becomes hard to see clearly on your own. That is where therapy for self-doubt may help. In CBT, the work is usually collaborative and practical. You look at the beliefs, habits, and triggers involved, then start testing them in a measured way.
The aim is not to build an inflated sense of confidence. It is to help you relate to doubt in a steadier, less fearful way so that your choices are not constantly being run by hesitation. For many people, that is where they begin to overcome self-doubt in a more lasting way.
Therapist Case Study: A Real-World Style Example
To protect privacy, we have anonymised the details of this client case while keeping the core pattern and therapy process true to the work.
When the client first made contact
A client came to therapy describing years of second-guessing herself at work and in relationships. She often rewrote emails, replayed conversations, and asked other people what they thought before trusting her own view. Outwardly, she seemed capable, but internally she felt tense, hesitant, and easily knocked by the possibility of getting things wrong.
The CBT method that was used
The early work focused on mapping the cycle. It became clear that self-doubt was strongest when she felt visible, responsible, or uncertain. Her mind quickly predicted criticism or failure, and she responded by overthinking, checking, and holding back. CBT then focused on testing those predictions through small behavioural experiments and reducing the habits that kept the doubt going.
Successful results
Over time, she became more able to make everyday decisions without lengthy review. She still noticed moments of doubt, but felt less controlled by them. What changed most was not that she felt certain all the time, but that she trusted herself more even when certainty was missing.
Final Thoughts
Self-doubt tends to loosen when you stop treating it as a verdict and start seeing it as a pattern. Overcoming self-doubt is often less about becoming completely confident and more about learning to make decisions, take action, and tolerate some uncertainty without letting it control you. Over time, that can help you build a steadier sense of trust in yourself, not because doubt disappears completely, but because it no longer gets to run the whole conversation.
FAQs
Is self-doubt the same as low confidence?
They are closely related, but not identical. Low confidence is often a broader feeling about your abilities, while self-doubt can show up as a repeating moment-to-moment pattern of questioning yourself, second-guessing decisions, and looking for certainty before acting.
Why does self-doubt get worse after mistakes?
Mistakes can activate beliefs such as “I am not capable”, “I am not good enough” or “I cannot trust myself.” When that happens, the mind may start reviewing, comparing, or checking for reassurance in an attempt to prevent the same thing from happening again.
Can overthinking make self-doubt worse?
Yes. Overthinking often feels like it should bring clarity, but it usually keeps your attention fixed on possible flaws, risks, or what-ifs. That can make you feel less settled and more scared in the future.
What does CBT actually do for self-doubt?
CBT helps you identify the triggers, beliefs, and behaviours that keep the pattern active. It then helps you test unhelpful predictions in real life, reduce safety behaviours (such as checking or reassurance-seeking), and build trust in yourself through repeated action.
Does progress mean never doubting yourself again?
No. The goal is not to remove every moment of uncertainty. The goal is to respond to doubt in a way that is less fearful, less controlling, and less likely to run your decisions for you.
Learn More
CBT for Menopause
A Comprehensive Guide to Managing Symptoms with Cognitive Behavioural Therapy (CBT)
Menopause is a natural biological process that every woman experiences. Yet, it often comes with a range of challenging symptoms that affect physical, emotional and mental wellbeing. Understanding the changes that occur during perimenopause and menopause is essential to navigating this transition with confidence. Cognitive behavioural therapy (CBT) offers an evidence-based approach to managing menopause symptoms improving mental health and enhancing quality of life.
What Happens in the Body During Perimenopause and Menopause?
Perimenopause:
Perimenopause, meaning “around menopause”, typically begins in a woman’s 40s but can start earlier. This phase can last anywhere from a few months to over a decade before menopause officially begins. It is marked by fluctuating oestrogen and progesterone levels, leading to irregular menstrual cycles and various physical and emotional symptoms.
Key hormonal changes during perimenopause include:
- Declining Oestrogen Levels: Affects mood, sleep, and bone health.
- Progesterone Reduction: Can lead to heavier or irregular periods and impact sleep patterns.
- Increased Follicle-Stimulating Hormone (FSH): Signals the ovaries to produce eggs but with inconsistent effectiveness, causing cycle irregularities.
- Changes in Testosterone: Can influence libido and energy levels.
Menopause:
Menopause is officially diagnosed when a woman has not had a period for 12 consecutive months. The average age of menopause is 51, but it can occur earlier due to genetics, medical conditions or surgical interventions, such as: hysterectomy.
During menopause:
- Ovaries stop producing significant amounts of estrogen and progesterone.
- The body adjusts to lower hormone level leading to a variety of symptoms.
- Risks of osteoporosis, cardiovascular disease and cognitive decline may increase.
Symptoms of Perimenopause and Menopause
The symptoms of perimenopause and menopause can be categorised into physiological, psychological, cognitive and behavioural changes. Below is a table outlining these symptoms:
| Category | Common Symptoms |
| Physiological | Hot flashes, night sweats, irregular periods, weight gain, vaginal dryness, headaches, joint pain, fatigue, changes in skin and hair |
| Psychological | Mood swings, increased anxiety, depression, irritability, feelings of sadness, emotional instability, low self-esteem |
| Cognitive | Brain fog, difficulty concentrating, forgetfulness, mental fatigue |
| Behavioural | Sleep disturbances, decreased libido, social withdrawal, increased stress responses, changes in eating and exercise habit |
How can Cognitive-Behavioural Therapy (CBT) improve quality of life?
Cognitive Behavioural Therapy (CBT) is a structured, evidence-based psychological therapy that helps individuals recognise and manage unhelpful thoughts and behaviours. CBT has been shown to be highly effective in reducing many menopause-related symptoms, particularly those related to mood, sleep and stress.
1. Managing Anxiety and Depression
Menopausal women often experience increased anxiety and depressive symptoms due to hormonal fluctuations. CBT helps by:
- Identifying negative thinking patterns and replacing them with balanced perspectives
- Using relaxation techniques, such as: controlled breathing and progressive muscle relaxation
- Developing problem-solving strategies to manage stress effectively
2. Coping with Hot Flashes and Night Sweats
Hot flashes and night sweats are among the most common and disruptive menopause symptoms. CBT can help by:
- Teaching mindfulness and acceptance strategies to reduce distress during hot flashes
- Encouraging lifestyle adjustments, such as: avoiding triggers like caffeine and alcohol
- Using cognitive re-structuring techniques to shift focus away from discomfort
3. Improving Sleep Quality
Insomnia and frequent night time awakenings are common during menopause. CBT for insomnia (CBT-I) is a specialised form of CBT that focuses on improving sleep by:
- Establishing a consistent bedtime routine and sleep schedule
- Reducing anxiety about sleep through cognitive re-framing
- Encouraging relaxation techniques and sleep hygiene improvements
4. Enhancing Cognitive Function
Brain fog and memory lapses can be frustrating symptoms of menopause. CBT can help by:
- Encouraging structured daily routines to improve focus
- Reducing cognitive overload through stress management strategies
5. Boosting Self-Confidence and Social Connection
Menopause can impact self-image and confidence. CBT helps by:
- Challenging negative self-perceptions and reinforcing positive affirmations
- Encouraging social engagement and support-seeking behaviours
- Helping women re-define their sense of purpose and self-worth beyond caring for others
Additional Lifestyle Strategies to Support CBT
While CBT is highly effective, combining it with lifestyle changes can further enhance wellbeing. Consider the following:
- Balanced Nutrition
- Regular Exercise
- Mindfulness and Meditation
- Social Support

Rebalance & Renew: A CBT Approach to Menopause
Rewrite Your Menopause Story. 6 Weeks. 10 Women. Real Strategies That Make a Difference.
Perimenopause and menopause are significant transitions in a woman’s life, often accompanied by physical, emotional and cognitive challenges. However, by understanding the physiological changes and utilising effective interventions, such as Cognitive Behavioural Therapy (CBT), women can regain control over their symptoms and improve their overall wellbeing.
This is the reason my experienced colleague, Ilia Maltezou, and I developed a 6-week online group programme for women going through (peri)menopause.
As we are both interested in women’s health, we wanted to create a safe space for women to share their experiences, receive and offer support and, of course, learn practical strategies that they can put in place to manage their distressing symptoms, navigate this period of change and improve their quality of life.
Our 6-week programme, based on the principles of Cognitive-Behavioural Therapy, covers the following areas:
- Identifying and managing physical symptoms of (peri)menopause
- Self-compassion and acceptance
- Identifying and managing unhelpful thoughts related to (peri)menopause
- Managing change
- Self-perception and identity shifts
- Using menopause as an opportunity for growth
- Developing a helpful routine that prioritises values
- Sleep hygiene and relaxation
Our programme will take place online. In this way, it will be more accessible to women in the UK. Every session will last for 90 minutes and the duration of the programme will be 6 weeks.
Following every session, we will provide participants with written materials that they can re-visit at any point during or after the end of the programme.
In regards to the cost, it is £510 for 6 weeks (£85 per 90-minute session).
Considering that nowadays we might pay around £85 for a massage or a facial that could last for less than 90 minutes, we really hope that women will also invest in their mental health in a similar way by attending our 6-week programme.
Sign up to our programme by e-mailing: therapyforme@outlook.com
Learn More
CBT for Health Anxiety
We have all heard of the term ‘health anxiety’ or ‘hypochondria’ and ‘hypochondriasis’ before. It is a term that we sometimes use lightly to suggest that we struggle with the idea of becoming unwell or we feel disgust and discomfort when we think about germs.
We have all felt concerned about our health at some point in our lives. It is likely that we have experienced urges to avoid medical procedures or medical professionals or to control the future by asking for reassurance and trying to predict the future. However, this is not an indication that we experience health anxiety or hypochondria.
What does ‘health anxiety disorder’ or ‘illness anxiety disorder’ mean in clinical terms? Who would meet the diagnostic criteria and what are the signs we might suffer from health anxiety?
Health anxiety symptoms:
1. Preoccupation with having or acquiring a serious illness
2. The preoccupation is excessive and disproportionate (even if a medical condition exists)
3. Excessive controlling or avoidant behaviours related to health (e.g. frequent visits to the GP, reassurance-seeking behaviours, researching symptoms on the internet but also avoiding talking about certain health conditions, avoid checking or touching parts of one’s body etc). In most cases, there is a mixture of controlling and avoidant behaviours and they can also co-exist and alternate (e.g. frequent visits to GP replaced by avoiding the GP)
4. Preoccupation for more than 6 months (even if the concerns change in content)
5. Preoccupation is not better explained by another mental disorder
I would like to clarify here that health anxiety is not just a preoccupation with our physical health. It can also be a preoccupation with our mental health – for example, the idea that one is losing their minds or developing psychosis or dementia.
Health anxiety can be diagnosed in people who already suffer from a medical condition or who have done in the past (in their childhood or early adulthood). It adds a layer of distress, anxiety and fear in their experience and it can be treated to improve their quality of life.
Health anxiety can be a debilitating condition – its severity ranges from mild to severe but when someone meets the diagnostic criteria for health anxiety, it means that their functioning is affected by the condition.
‘Health anxiety is ruining my life! Can I stop health anxiety?’
Health anxiety disorder is indeed a condition that can have a serious impact on people’s lives, routines, relationships…it can affect all life areas. Cognitive-behavioural therapy is an evidence-based treatment for health anxiety. Unfortunately, it won’t make the health anxiety stop but it will teach you important strategies for you to start managing your health anxiety symptoms better and start taking back the control from your anxiety.
‘’How can CBT help with health anxiety? How can I handle health anxiety? What can I expect from health anxiety treatment using the CBT model?’’
First of all, let’s think what it is realistic to expect from health anxiety therapy. Many people come to therapy expecting their worry thoughts and anxiety to go away. However, although we would expect that CBT therapy will help with the reduction in anxiety and worry symptoms in the long-term, it is unrealistic to expect that such thoughts and feelings will disappear forever. As human beings it is natural and expected to experience difficult thoughts and emotions at certain points in our lives.
CBT therapy does not aim to reduce the uncertainty that the future brings or rule out the possibility of a medical condition. These would be unrealistic expectations. CBT therapy for health anxiety aims to help the person tolerate uncertainty and find better ways in managing their distress and difficult thoughts through:
– Educating the person about how anxiety and fear affect the body and lead to distressing physical sensations. Some people ask whether health anxiety can cause ‘fake symptoms’. The answer is that anxiety activates the ‘fight-or-flight’ response in our bodies leading to new symptoms that could be perceived as dangerous and an indication of a serious health condition. For example:

– Working with the catastrophic misinterpretations that the person is led to when interpreting new or ambiguous physical symptoms.
– Helping the person identify rigid and unhelpful thinking styles. Working on reinforcing flexibility in the way situations are interpreted.
– Encouraging the person in therapy to test out negative predictions through engaging with distressing thoughts, feelings and scenarios.
– Teaching the person how to focus their attention on what they find meaningful and in line with their values, rather than what their anxiety directs them to.
– Postponing unhelpful behaviours which reinforce the anxiety in the long-term, such as: checking, asking for reassurance and monitoring symptoms excessively.
– Liaising with the GP in order to develop a joint plan that would benefit the person.
– Working with the family of the individual to educate them on health anxiety and make sure they do not unintentionally reinforce health anxiety symptoms.
– Helping the person reduce avoidant behaviours as a way of building self-confidence and self-esteem and reducing fear and anxiety.
Health anxiety by proxy
When individuals are preoccupied with the health of someone else (e.g. their children) and they experience the health anxiety symptoms we referred to in the beginning of this article, they could be diagnosed with health anxiety by proxy. The treatment for this type of health anxiety would involve the same processes and the aim of therapy would be exactly the same as the above description.
Books recommended for health anxiety
Overcoming Health Anxiety: A self-help guide using cognitive behavioural techniques (2009) by David Veale and Rob Willson
Learn More
Idyli Kamaterou on BBC radio for Stress Awareness Month
”Stress Awareness Month has been held every April, since 1992. During this annual thirty day period, health care professionals and health promotion experts across the country will join forces to increase public awareness about both the causes and cures for our modern stress epidemic”.
This year, as part of the Stress Awareness Month, Idyli Kamaterou from Therapy For Me attended an interview on BBC radio. During this interview we talked about areas, such as:
• Symptoms of stress that we should all monitor in our lives
• Support available for people who experience stress
• Causes of stress in adults under 35 years old
• What Cognitive -Behavioural Therapy is and how it can help people manage stress
If you work in a charity or organisation that might be interested in discussing adult mental health, please contact us. It would be our pleasure to organise a workshop and continue raising awareness.
Learn More